| UW MSK Resident Projects |
|
|
|
|
Neuropathic Joint DiseasePrint-friendly version of this pagePosted by fauxbohemian@yahoo.com, 1/5/04 at 8:41:12 AM.
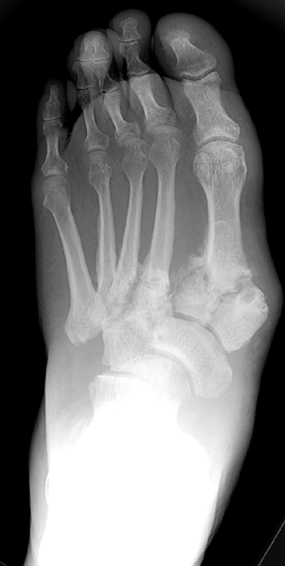
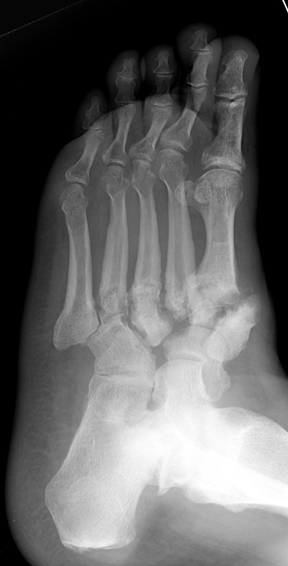
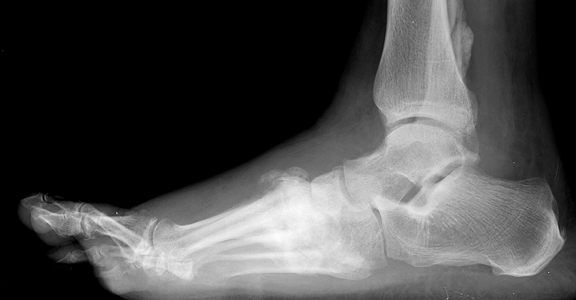
Neuropathic Joint Disease January 7, 2004 Top Ten Things a Curious Resident Could Ask About Neuropathic (Charcot) Joint Disease... 10. Who is Charcot and why is there a joint named after him? Jean-Martin Charcot was a French neurologist (of course) who in 1868 recognized a link between neurosyphilis (tabes dorsalis) and a particular kind of deformed joint. Initially he thought the deformity was due to "spontaneous fracture," but he eventually realized that it may be a chronic process related to the neuropathy itself. Since then, numerous scientists have advanced theories explaining why certain neuropathies give rise to abnormal joints. In 1936, physicians first formally posited a link between diabetes mellitus and the so-called "Charcot joint." 9. What exactly is a neuropathic arthropathy? This term refers to progressive degeneration of a weight-bearing joint, a process marked by bony destruction, bone resorption, and eventual deformity. Onset is usually insidious. 8. What types of conditions give rise to neuropathic joint? Basically, any condition resulting in decreased peripheral sensation, proprioception, and fine motor control: * Diabetes mellitus neuropathy (the most common in the U.S. today, resulting in destruction of foot and ankle joints), with Charcot joints in 1/600-700 diabetics. Related to long-term poor glucose control. * Alcoholic neuropathy * Cerebral palsy * Leprosy * Syphilis (tabes dorsalis), caused by the organism Treponema pallidum * Congenital insensitivity to pain * Spinal cord injury * Myelomeningocele * Syringomyelia * Intra-articular steroid injections 7. What are the underlying mechanisms responsible for the neuropathic joint? Two primary theories have been advanced: * Neurotrauma: Loss of peripheral sensation and proprioception leads to repetitive "microtrauma" to the joint in question; this damages goes unnoticed by the neuropathic patient, and the resultant inflammatory resorption of traumatized bone renders that region weak and susceptible to further trauma. Indeed, it is a "vicious cycle." In addition, poor fine motor control generates unnatural pressure on certain joints, leading to additional microtrauma. *Neurovascular: Neuropathic patients have dysregulated autonomic nervous system reflexes, and de-sensitized joints receive significantly greater blood flow. The resulting hyperemia leads to increased osteoclastic resorption of bone, and this, in concert with mechanical stress, leads to bony destruction. In reality, both of these theories probably play a role in the development of a Charcot joint. 6. OK, enough yakking about pathogenesis - what joints as a radiologist should I be worried about? As diabetes is the #1 cause in America today for neuropathic joint disease, the foot is the most affected region. In those with foot deformity, approximately 60% are in the TMT joint (medial > lateral), 30% MCP joint, and 10% have ankle disease. Over half of diabetic patients with neuropathic joints can recall some kind of precipitating trauma, usually minor. Patients with neurosyphilis tend to have knee involvement, and patients with syringomyelia of the spinal cord may demonstrate shoulder deformity. Hip joint destruction is also seen in neuropathic patients. 5. Now we can get to the good stuff. What kind of radiographic findings can we expect with this insidious process? First, it is important to recognize that two types of abnormality may be detected. One is termed "atrophic," in which there is osteolysis of the distal metatarsals in the forefoot. The more common form of destruction is "hypertrophic" joint disease, characterized by acute peri-articular fracture and joint dislocation. The natural history of the joint destruction process has a classification scheme of its own, offered by Eichenholtz decades ago: Stage 0: Clinically, there is joint edema, but radiographs are negative. Note that a bone scan may be positive before a radiograph is, making it a sensitive but not very specific modality. Stage 1: Osseous fragmentation with joint dislocation seen on radiograph ("acute Charcot"). Stage 2: Decreased local edema, with coalescence of fragments and absorption of fine bone debris Stage 3: No local edema, with consolidation and remodeling (albeit deformed) of fracture fragments. The foot is now stable. 4. What is the clinical presentation, by the way? Erythema, edema, increased temperature in the affected joint. In neuropathic foot joints, plantar ulcers may be present. Note that it is often difficult to differentiate osteomyelitis from a Charcot joint, as they may have similar tagged WBC scan and MRI features (joint destruction, dislocation, edema). Definitive diagnosis may require bone or synovial biopsy. 3. Is Charcot joint serious? Well, if this pathological process continues unchecked, it could result in joint deformity, ulceration +/- superinfection, loss of function, and in the worst case scenario: amputation. Early identification of joint changes is the best way to limit morbidity. 2. How is it treated? Once the process is recognized, immobilization with a total contact cast will help ward off further joint destruction. Pneumatic walking braces are also used. Surgical correction of a joint is rarely successful in the long-term in these patients. It can take 6-9 months for the edema and erythema of the affected joint to recede. 1. Finally, can you show us a picture of a Charcot joint?
Destroyed TMT joints in the medial left foot, with fracture and dislocation of fragments; these are classic findings. Also note loss of the foot arch and acquired pes planus deformity (images courtesy of Dr. John Hunter's teaching file). References 1. Canale: Campbell's Orthopaedics, 10th edition, 2003 Mosby, Inc. 2. Gupta, R. 1993. A short history of neuropathic arthropathy. Clinical Orthopaedics, 296, pp. 43-49. 3. Sommer, Todd C., and Lee, Thomas H. Charcot Foot: The Diagnostic Dilemma. American Family Physician. Vol. 64, No. 9, Nov. 1, 2001.
|
|